ClimaSalud-IA
climate change, extreme heat, chronic disease, AI, predictive model, heatwave, Mútua Terrassa, Meteocat, epidemiology, case-crossover, UPC
| Full title | ClimaSalud-IA: AI for extreme climate events and chronic disease risk |
| Status | Active · hospital pilot phase |
| Clinical partner | Mútua Terrassa University Hospital |
| Meteorological partner | Meteocat — Servei Meteorològic de Catalunya |
| University | Universitat Politècnica de Catalunya (UPC / IRIS) |
| B2SLab PI | Alexandre Perera Lluna |
Context: climate change and chronic disease
Climate change is not a future risk for healthcare systems — it is a present one. Extreme heat events are intensifying in frequency, duration, and severity across Europe, and the Mediterranean region is warming faster than the global average. For Catalonia’s ageing population, where more than half of residents live with at least one chronic condition, each heat episode represents a direct clinical threat.
The physiological challenge is straightforward: the human body maintains core temperature within a narrow range (37 ± 0.5 °C). Extreme heat impairs thermoregulatory capacity, triggering a cascade of effects — dehydration, cardiovascular strain, renal stress, endothelial dysfunction — that interact with the vulnerabilities of pre-existing disease. The result is measurable, and preventable, excess morbidity and mortality during heat episodes.
What was missing, until ClimaSalud-IA, was the quantitative epidemiological foundation and the AI infrastructure to translate that knowledge into prospective clinical action.
The research: heat exposure and health-care use
In collaboration with Mútua Terrassa University Hospital and Meteocat, B2SLab conducted a detailed epidemiological study of the short-term association between heat exposure and four health outcomes in the hospital’s patient population:
- Mortality
- Emergency department visits
- Hospital admissions
- Unplanned primary care visits
Study population
The analysis drew on linked administrative and clinical data from Mútua Terrassa and the Catalan public health system (eCap / CatSalut), covering the municipalities served by the hospital across the Vallès Occidental area.
| Outcome | Total events | ≥65 years | Cardiovascular comorbidity |
|---|---|---|---|
| Death | 1,791 | 87.0% | 65.3% |
| Emergency visit | 134,566 | 26.8% | 39.1% |
| Hospital admission | 17,840 | 50.1% | 58.8% |
| Unplanned primary care | 34,329 | 26.6% | 38.9% |
Patients were classified into eight comorbidity groups based on their diagnoses:
| Comorbidity group | Included diagnoses |
|---|---|
| Cardiovascular | Congestive heart failure; myocardial infarction; peripheral vascular disease; cerebrovascular disease; arrhythmias |
| Respiratory | Chronic pulmonary disease; asthma |
| Endocrine-metabolic | Diabetes mellitus; liver disease; thyroid disorders |
| Renal | Chronic renal disease |
| Mental-psychiatric | Depression; anxiety; psychotic disorders; bipolar disorder |
| Neurological | Dementia; Parkinson’s disease |
| Cancer-immunologic | Solid or haematological malignancy; metastatic cancer; HIV/AIDS |
| Rheumatic-inflammatory | Rheumatic disease |
Heat definition
There is no globally standardised definition of heat, and the choice of definition has material consequences for epidemiological analysis. The study used the operational thresholds of Meteocat, the Catalan Meteorological Service, which grounds heat alerts in the local climatological baseline:
Statistical method: case-crossover design
The study applied a time-stratified case-crossover design, which controls for confounding by stable individual characteristics by comparing the heat exposure preceding each health event to exposure on matched control days within the same calendar month. This approach isolates the transient effect of heat without requiring an unexposed control population.
Four alternative exposure definitions were compared to assess the sensitivity of results to methodological choices about how heat is measured:
- A. Single-day exposure — temperature at a single lag day
- B. Window-averaged exposure — mean temperature over a 3-day window (lags 5–7)
- C. Finite memory exposure — mean temperature over the 6 preceding days (lags 0–5)
- D. Decaying exposure — exponentially weighted temperature over 15 days, with a fitted half-life
Key finding: distinct temporal associations
The implication for clinical prediction is direct: a heat wave management system that monitors only the preceding 1–2 days will capture mortality risk but will systematically miss the excess primary care burden, which accumulates over nearly two weeks of sustained heat. An effective early warning system must account for this heterogeneity.
Across all outcomes and exposure definitions, a 1 °C increase in heat exposure was associated with significant increases in all four healthcare outcomes, with the strongest effects in mortality (OR ~1.06–1.08 per 1 °C increase, short lags) and hospital admissions. Among comorbidity groups, neurological disease showed the sharpest hospital admission risk at lags 0–4 days, while cardiovascular and endocrine-metabolic groups showed consistent effects across all outcomes.
The ClimaSalud-IA platform
Building on this epidemiological evidence, B2SLab designed and implemented ClimaSalud-IA — an AI platform that integrates heterogeneous data streams to anticipate the clinical impact of heat episodes prospectively.
The predictive model uses the temporal association structure identified in the epidemiological study — applying outcome-specific exposure windows so that mortality risk, hospitalisation risk, and primary care demand are each modelled at their own appropriate time scale.
Dashboard
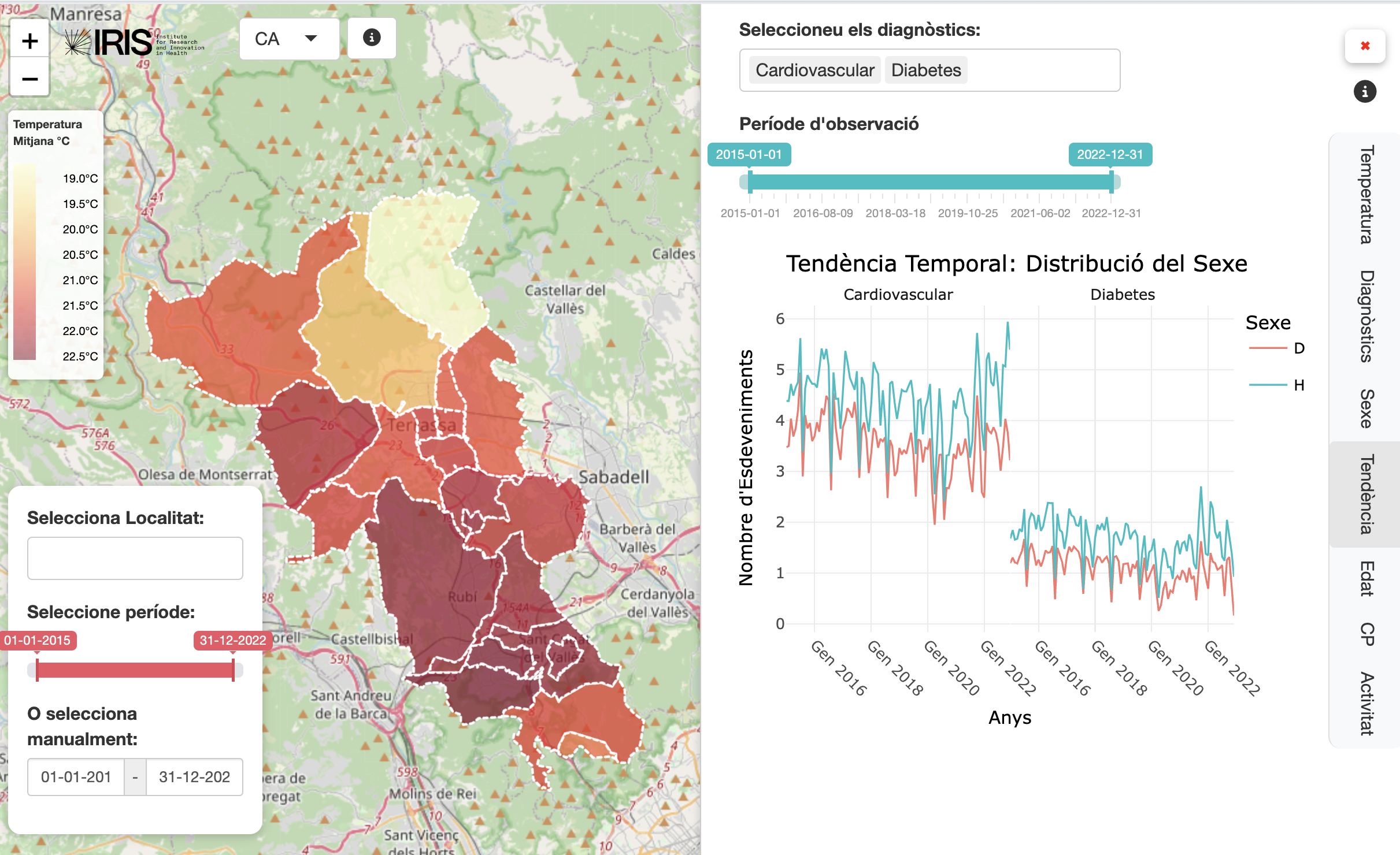
The platform includes a clinical decision support interface designed for hospital and primary care management teams. During heat episodes, the dashboard surfaces:
- Patients at elevated risk by comorbidity group and age band
- Expected demand increase by care level (primary care, emergency, hospital)
- Temporal trajectory of risk over the coming days
Hospital pilot: Mútua Terrassa
The hospital pilot at Mútua Terrassa University Hospital is the current phase of the project. Its objectives are to:
- Connect the platform to live hospital and CatSalut data in a compliant, secure configuration
- Complete final model training with post-2022 patient data, including cost-of-care dimensions
- Train clinical and operational staff
- Collect prospective data on clinical utility and operational impact during the 2026 heat season
- Document the results as the evidence base for territorial expansion
All activities are conducted in compliance with the General Data Protection Regulation (GDPR) and Catalan digital health regulations.
Funding and partners
ClimaSalud-IA is an active collaboration between:
- B2SLab / IRIS-UPC — AI methodology, epidemiological analysis, platform design
- Mútua Terrassa University Hospital — clinical partner, data access, pilot deployment
- Meteocat — Servei Meteorològic de Catalunya — meteorological data and heat alert thresholds